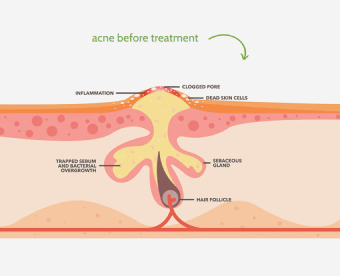
Dermatologists, or doctors who treat skin conditions, are often thought of as an essential part of any acne treatment plan. But is this really the case? Dermatologists will likely default to offering you a prescription whether or not you really need it.
Dermatologists are trained to treat acne by prescribing medications, but they may over-prescribe medication, or even give medication to people who don't really need it. Dermatologists will give prescriptions for higher concentration topical medications or even hormonal treatments like birth control or Spironolactone. Much of the time, over-the-counter topical treatments work better than these more aggressive treatment plans, so you should try those before resorting to a pricey and time-consuming dermatologist.
It is important to consider other, gentler ways to treat acne, such as a balanced skin care regimen. Cleansers, tonics, and serums will treat your acne without risking the detrimental side effects that can come with a prescription.
Also read: How to choose the best acne treatment

What is a Dermatologist?
According to the American Academy of Dermatology, a dermatologist is a doctor who specializes in skin, hair, and nail conditions and treatment. Under this umbrella is acne, one of the most prevalent health conditions in the world.
A dermatologist will complete approximately 12 years of training in order to become board certified, including undergraduate education, medical school, and residency. From there, they can begin to treat acne.
A Dermatologist's Treatment Plan
A common misconception is that a dermatologists' job is to treat acne. But dermatologists are trained to prescribe medication, even if you do not need it, and even if those medications come with severe side effects.
A dermatologist's treatment plan will typically consist of one or several of the following medications:
-
Retinoids
-
Azelaic acid
-
Benzoyl peroxide
-
Salicylic acid
-
Hormonal therapy
-
Isotretinoin (commonly referred to as Accutane)
Many of these medications are very aggressive and can lead to negative side effects.
Pros of Prescriptions
You likely only need to see a dermatologist if you're experiencing severe acne symptoms such as cysts or nodes that can be more difficult to treat and identify. Cystic acne is incredibly rare and because it is so uncommon, most people experiencing acne should not need a dermatologist.
How to identify cystic acne:
-
The acne is leading to permanent scarring, such as skin discoloration or craters in the skin
-
The acne is deep under your skin
-
Your acne is itchy, painful, or burning, sometimes even when you do not touch it
In addition, doctors can often prescribe more concentrated versions of effective topical treatments like azelaic acid, benzoyl peroxide, and salicylic acid. Over-the-counter treatments often contain these same ingredients at less harsh concentrations.
With that being said, our treatment here at Exposed has been proven to work against serious, cystic acne. So before spending the time and money on a doctor, try out our topical treatments and enjoy the benefits without worrisome side effects.

Cons of Prescriptions
Despite there may be certain reasons to seek out a dermatologist for acne treatment, there are also negatives, including:
-
Aggressive treatment plans
-
Medications with negative side effects
-
Negligence of cheaper, effective, OTC treatments
-
Time-consuming, often requires various trips to the dermatologist as they trial-and-error their way through treatment plans
-
Going to a dermatologist is very expensive, especially because many insurance plans don't cover skin care
Instead of going to a dermatologist, your acne can simply be treated with gentle, topical products like cleansers and moisturizers- you just need to find the right combination.
Therefore, much of the time, the medications a dermatologist could provide may be too aggressive for most people's acne.
In addition, the medications that doctors provide will often come with negative side effects. For example, the leading treatment for severe acne, isotretinoin, causes severe birth defects and can be a risk to anyone who can become pregnant while taking it.
Another one of the most common prescriptions given by dermatologists is a topical antibiotic, which is meant to curb the overgrowth of P. acnes bacteria. Nonetheless, it is possible to develop antibiotic resistance wherein the medication ceases to be effective as bacteria develop the ability to defeat the antibiotic.
Finally, when you go to a dermatologist to get a prescription, they will likely neglect to recommend any useful over-the-counter treatments that will drastically improve your acne alone. For this reason, examine your options with over-the-counter regimens before seeing a dermatologist.
How to Get Rid of Acne with the Exposed Skincare Routine
The first step to treating acne should always be an easily accessible, over-the-counter acne treatment regimen.
At Exposed Skincare, we know that topical acne treatments are the most effective way to achieve clearer skin without unpleasant side effects. We utilize dermatologist-trusted ingredients such as benzoyl peroxide, azelaic acid, and salicylic acid in appropriate concentrations that won't irritate.
We also add soothing, natural derivatives like green tea extract, passion flower extract, and pumpkin seed extract to calm inflammation and moisturize.
Here's how it works:
-
In the morning, you start off with a gentle cleanser to clear away any excess oil from the night.
-
After that, you apply a thin layer of toner that will learn and open your pores to prepare them to receive more treatment.
-
You then will apply the acne treatment serum, allowing it to sink into your freshly cleansed pores.
-
You'll then apply a moisturizer that makes your skin look supple and fresh for the day.
-
As a final step in the morning, you'll take a probiotic supplement that helps gut health and introduces ingredients that your body can use to fight acne.
-
And in the evening, you'll cleanse and use your tonic again to clear away any contaminants from the course of your day.
-
Then, before you sleep, you'll apply the clean pore serum that ensures you won't develop any clogged pores during the night, and, if you have dry skin, another layer of moisturizer.
-
Two times a week, you will use the Microderm scrub that exfoliates excess dead skin cells.
-
And twice a week you will also apply a soothing, clarifying sulfur mask.
And after a month of keeping with your routine? You will see a major reduction in your acne. In fact, we guarantee it.
If you are thinking about going to a dermatologist for acne, we know that you may feel frustrated and worry that a dermatologist is your final option. But we're here to tell you that Exposed works, and it works without all the side effects and lost money that you have to deal with when going to a dermatologist.
So browse our options, and find out why thousands of people finally found an answer to their acne with Exposed.