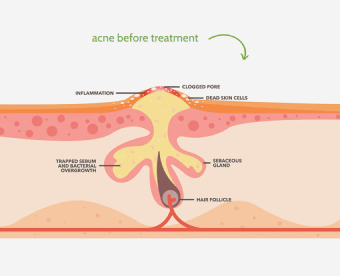
Antibiotics were once the golden ticket for acne, but they're quickly losing their magic touch. With over 50% of acne bacteria now giving these meds the middle finger, dermatologists are pumping the brakes on prescriptions. The side effects aren't exactly a walk in the park either—gut issues, yeast infections, and contributing to superbugs? No thanks. Exposed Skin Care's antibiotic-free system tackles acne from multiple angles, with results that might make you question why you ever popped those pills.
Biggest Takeaways
- Antibiotic resistance has increased from 20% to over 50% in acne bacteria since the 1970s.
- Dermatologists prescribe 5% of all antibiotics despite being only 1% of doctors.
- Antibiotics can cause side effects from skin irritation to gut microbiome disruption that takes years to recover.
- Current medical guidelines recommend limiting antibiotic use to three months and pairing with other treatments.
- Exposed Skin Care offers a non-antibiotic alternative targeting all four acne causes with clinically proven results.
Understanding Antibiotics and Their Role in Acne Treatment

When you're dealing with stubborn acne that just won't quit, antibiotics often enter the conversation as a potential solution.
In the debate on antibiotics for acne, they're typically reserved for severe cases that laugh in the face of your typical topical treatments.
Here's the deal: antibiotics like doxycycline and minocycline work by targeting the bacteria causing your breakouts while calming inflammation.
But they're not some miracle cure you should casually pop – over 50% of acne bacteria strains have developed resistance to certain antibiotics.
That's why dermatologists are getting pickier about prescribing them.
They work best when paired with topical treatments (never solo), and ideally shouldn't be used longer than three months.
Think of antibiotics as the backup dancer, not the main event in your acne-fighting routine.
The Growing Concern of Antibiotic Resistance in Skincare
Three alarming stats you won't hear from your dermatologist: antibiotic resistance in acne bacteria has skyrocketed from 20% in 1978 to over 50% today.
Derms prescribe 5% of all antibiotics despite making up just 1% of doctors, and those cute little tubes of topical antibiotics are creating superbugs that laugh at our medicine cabinet.
Yikes. The American Academy of Dermatology is finally catching up, now warning against using antibiotics alone.
Even major medical authorities now admit the antibiotics-only approach to acne treatment has been dangerously misguided.
But how many of us have been handed a prescription with zero explanation about resistance risks?
This isn't just about your face—it's about everyone's future health.
When antibiotics stop working for acne, they might fail when you really need them for something serious.
Smart skincare means targeting all four acne drivers without antibiotics' long-term risks.
Common Side Effects of Antibiotics for Acne Management

Those "miracle" antibiotic prescriptions for acne don't come without their share of baggage.
While your dermatologist might make them sound like the holy grail, your body often has different plans.
Slap on topical antibiotics and you're signing up for potential dryness, irritation, and that lovely flaky skin look nobody asked for.
Pop oral antibiotics, and you might be racing to the bathroom with nausea, diarrhea, or dealing with a surprise yeast infection (fun times!).
Let's talk long-term fallout: antibiotic resistance isn't just science talk—it means these meds stop working when you actually need them.
Even worse, your gut microbiome gets totally wrecked, potentially taking years to bounce back.
With over half of acne bacteria already resistant to common treatments, maybe it's time to question if this solution is actually creating bigger problems.
Why Many Dermatologists Are Scaling Back Antibiotic Prescriptions
The medical community's romance with antibiotic acne treatments is cooling faster than yesterday's coffee.
Those prescription pads aren't getting whipped out like they used to—and for good reason.
Here's why your derm might be pumping the brakes on antibiotics:
-
Over 50% of acne bacteria are now giving antibiotics the middle finger
-
Resistance has tripled since the 70s (from 20% to a whopping 62%)
-
Derms make up a tiny slice of doctors but write nearly 5% of all antibiotic scripts
-
The big-shot Global Alliance says ditch topical antibiotics after three months
-
Combining antibiotics with benzoyl peroxide or retinoids is now the move, not solo antibiotic therapy
You're not alone in this frustrating skin battle—but your solution doesn't have to come with a resistance problem attached.
The Multi-Driver Approach: Why Exposed Skin Care Works Differently

While antibiotics are becoming tomorrow's flip phones in the acne treatment world, smarter solutions have been quietly gaining traction.
Enter Exposed Skin Care's multi-driver approach – the skincare equivalent of hitting acne with a well-coordinated SWAT team instead of a lone security guard.
Multi-pronged acne attacks work better than solo agents – like sending in special forces when a mall cop won't cut it.
Unlike one-note treatments that only target bacteria (hello, antibiotic resistance!), Exposed tackles all four acne culprits simultaneously: excess oil, clogged pores, bacteria, and inflammation.
Their Basic Kit isn't just throwing random ingredients at your face – it's a calculated system where each product plays its role in the acne-fighting orchestra.
The proof? Over 1,000 five-star reviews from people who've ditched their dermatologists' prescriptions.
With customizable routines and science-backed ingredients, you're not just treating symptoms – you're addressing root causes without creating superbugs on your face.
Clinical Results: How Exposed's System Outperforms Antibiotic-Only Options
When clinical studies pit Exposed's multi-ingredient system against conventional antibiotic treatments, the numbers tell a story antibiotics can't match.
While antibiotics take their sweet time and sometimes ghost you completely, Exposed users typically see real improvements in weeks, not months.
What makes Exposed the clear winner? Let's break it down:
-
Tackles all four acne drivers simultaneously, not just the bacteria part
-
Zero antibiotic resistance issues (because, duh, no antibiotics)
-
Over 1,000 five-star reviews from actual humans with formerly angry skin
-
Noticeably fewer relapses compared to the antibiotic roller coaster
-
No weird side effects like the stomach issues antibiotics love to cause
You're not just treating symptoms—you're fixing the whole problem, which explains why so many Exposed users leave the antibiotic merry-go-round behind for good.
Real Customer Transformations With Exposed's 3-Step System
Instead of taking our word for it that Exposed works better than antibiotics, let's look at actual humans who've ditched the pills for our 3-step system.
Over 1,000 five-star reviews tell the same story: people with stubborn acne finally seeing clear skin within weeks—not the months typical antibiotics take.
And we're not talking about just fewer pimples (though that happens too). Users rave about improved texture, reduced redness, and that confidence boost when you're not constantly worrying about your skin.
What makes these transformations legit is how our system tackles all four acne drivers simultaneously, not just bacteria.
While antibiotics focus on one factor, Exposed's blend of clinical actives and botanicals works on excess oil, clogged pores, and inflammation too—without the gut issues antibiotics bring.
Breaking the Acne Cycle: Creating a Sustainable Skincare Routine
Breaking the cycle of endless acne flare-ups requires more than just dabbing on random products whenever you feel like it.
You need a consistent routine that tackles all your skin's issues simultaneously—not just the zits you can see.
Here's what actually works to keep your face clear long-term:
-
Cleanse gently but daily—harsh scrubbing just pisses off your skin
-
Include acne-fighting ingredients (salicylic acid or benzoyl peroxide) that actually work, not trendy "miracle" extracts
-
Don't skip moisturizer—dry skin overproduces oil, creating more breakouts
-
Exfoliate 1-2 times weekly to kick those dead cells to the curb
-
Watch what you eat—those sugary snacks might be sabotaging your skin game
Consistency is key.
Your skin doesn't clear up overnight, so stick with it!
Frequently Asked Questions
How Long to See Results of Antibiotic Acne?
You'll typically notice improvements in 2-4 weeks, but full antibiotic effects take 6-12 weeks. Meanwhile, Exposed's complete system tackles all four acne drivers for faster, more reliable results.
Is It a Good Idea to Take Antibiotics for Acne?
Antibiotics can help severe acne, but you'll face potential side effects and resistance risks. Instead, try Exposed's complete system that targets all four acne drivers without antibiotic drawbacks or rebound breakouts.
Why Did My Acne Go Away With Antibiotics?
Your acne improved because antibiotics targeted the bacteria driver of acne. They're effective short-term, but won't address sebum, clogged pores, or lasting inflammation—that's why breakouts often return.
Why Are Medical Professionals Reducing the Use of Antibiotic Treatment for Acne?
Medical professionals are reducing antibiotic use for acne because bacteria are becoming resistant. They've seen resistance rates jump from 20% to over 50%, making your treatment less effective over time.
Putting It All Together
You're done riding the antibiotic rollercoaster for acne. While prescriptions might temporarily tame your breakouts, they're just putting a band-aid on a four-headed monster. Exposed's system tackles all your acne drivers simultaneously, giving you sustainable results without the resistance concerns or side effects. Why settle for partial solutions when you can address the whole problem? Your skin deserves more than just bacteria-fighting—it needs thorough care that actually sticks around.