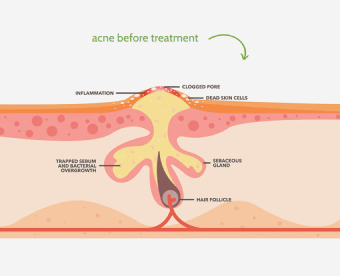
Fungal acne, also known as Malassezia folliculitis, is a common skin condition that affects many people.
Unlike regular acne, which is caused by the accumulation of sebum and bacteria in the pores, fungal acne is caused by the overgrowth of yeast on the skin. Fungal acne can be frustrating and uncomfortable, but effective treatment is possible.
Also read: How to choose the best acne treatment
Biggest Take-Aways:
-
Fungal acne appears as small, itchy, red bumps on the skin that do not respond well to most traditional acne treatments and is caused by an overgrowth of yeast on the skin.
-
Prevention tips include keeping the skin clean and dry, wearing loose-fitting clothing, and avoiding oily or greasy products.
-
Fungal acne can be effectively treated and managed, but it may not be curable, and consulting with a dermatologist is recommended to determine the best treatment plan.
-
Effective treatment options for fungal acne include antifungal topical and oral medications and natural remedies such as tea tree oil.

Symptoms of Fungal Acne
Fungal acne appears as small, itchy, red bumps on the skin that do not respond to traditional acne treatments. The bumps are typically uniform in size and shape, and they may occur in clusters.
Fungal acne is commonly found on the chest, back, and upper arms, but it can occur anywhere on the body.
Causes of Fungal Acne
Fungal acne is skin infection caused by an overgrowth of a type of yeast called Malassezia on the skin. This yeast is found on the skin of almost everyone, but in some people, it can overgrow and cause skin problems.
Factors that increase the risk of developing a fungal infection or acne include a humid environment, a weakened immune system, and the use of certain medications.
Fungal Acne Treatment Options
Antifungal topical treatments
Topical antifungal agents, such as Ketoconazole and Ciclopirox, are effective in treating fungal acne.
These agents work by killing the yeast that is causing the acne. Some over-the-counter antifungal creams can be used for fungal acne treatment, but it is best to consult a dermatologist for a prescription-strength product.
Antifungal oral treatments
Oral antifungal medications, such as Itraconazole and Terbinafine, are effective in treating severe cases of fungal acne.
These medications work by killing the yeast from the inside out. Oral antifungal medications may have some side effects, so it is important to consult a dermatologist before starting treatment with oral antifungal medication.

Natural remedies
Kumar 2012 found that cow urine, lemon, boiled rice water, and Neem extract are effective in curing dandruff and inhibiting the growth of the causative fungus Malassezia.
-
The study conducted a comparison of natural remedies such as cow's urine, lemon juice, boiled rice water, and Neem extract to cure dandruff.
-
Modified Oil - Potato Dextrose Agar was used as the nutrient medium for fungal growth in this experiment.
-
Cow's Urine proved to be more stable and effective than other treatments while Boiled Rice Water also showed good results against Malassezia fungus which causes Dandruff.
-
Lemon Juice had high effectiveness but only over a shorter period of time compared with others.

Martin 2004 found that tea tree oil, Solanum species, and oil of bitter orange preparations showed encouraging results in clinical trials.
-
The systematic review evaluated antifungal herbal preparations that have been tested in controlled clinical trials.
-
Tea tree oil was the most thoroughly clinically tested and showed some promise as an antifungal medicine.
-
Solanum species (two trials) and oil of bitter orange preparations (one trial) were also compared with conventional treatments, showing encouraging results.
-
All herbal remedies require further investigation in rigorous clinical trials to confirm their efficacy for treating fungal infections
KAUSHIK 2019 found that natural medicines of plant origin are still used as therapeutic agents, especially for treating bacterial, fungal, viral, protozoal, helminthic infections, etc.
-
Various antifungal agents such as azoles, allylamines, echinocandins, etc., are used clinically for treating these kinds of infection but drug resistances remain an issue with them.
-
Plant constituents offer great promise when it comes to preventing/treating systemic fungal infections due to their chemical diversity; hence there is huge potential here for new drug development based on natural compounds
These findings suggest that natural remedies can be effective in treating fungal acne.
Prevention Tips
Keep the skin clean and dry
Fungal acne thrives in warm, humid climates and otherwise moist environments, so it is important to keep the skin clean and dry.

Wear loose-fitting clothing
Tight clothing can trap moisture against the skin, creating an environment where the yeast can thrive. Wear loose-fitting clothing made of breathable fabrics to prevent yeast growth and prevent fungal acne.
Avoid oily or greasy products
Oil-based products can contribute to the development of fungal and bacterial acne too. Choose products that are labeled as non-comedogenic, which means they will not clog pores.
Conclusion
Fungal acne is a frustrating and uncomfortable skin condition, but effective treatment is possible. By consulting with a dermatologist, you can determine the best treatment for your specific case of fungal acne.
Natural remedies may provide some relief, especially tea tree oil.
Prescription-strength antifungal medications are the most effective solution, though. What direction you take depends on the severity of the infection.
It is also important to follow proper prevention tips to avoid the development of fungal acne. Keeping the skin clean and dry, wearing loose-fitting clothing, and avoiding oily or greasy products can help reduce your risk.
If you are experiencing symptoms of fungal acne, do not hesitate to consult a dermatologist. With the right treatment and prevention measures, you can effectively manage this common skin condition.

Fungal Acne Treatment FAQs
Does oily skin make you more prone to fungal acne?
Yes, oily skin can make you more prone to developing fungal acne. The yeast that causes fungal acne, Malassezia, thrives in environments that are warm and moist, and excess oil on the skin can provide the perfect breeding ground for yeast infection.
What makes fungal acne worse?
Fungal acne can be worsened by a number of factors, including hot and humid weather, excessive sweating, use of occlusive skin care products, and certain medications such as steroids.
How is fungal acne diagnosed?
Fungal acne is diagnosed through a physical examination of the skin by a dermatologist, and by taking a skin scraping for microscopic analysis.

Why do fungal infections occur?
Fungal infections, including fungal acne, occur when the balance of microorganisms on the skin is disrupted. This can happen due to factors such as excessive sweating, use of antibiotics, or changes in the skin's pH.
How long does it take for fungal acne to clear up?
The length of time it takes for fungal acne to clear up can vary depending on the severity of the condition and the chosen treatment method. It may take several weeks or even months to see improvement.
Can fungal acne be cured?
Fungal acne can be effectively treated and managed, but it may not be curable. It is important to follow proper skin care hygiene and avoid triggers that can cause the condition to flare up.
Is fungal acne the same as acne vulgaris?
No, fungal acne is not the same as acne vulgaris. While they may appear similar to regular acne on the surface, fungal acne is caused by an overgrowth of the yeast Malassezia on the skin, while typical acne vulgaris is caused by an overproduction of sebum and bacterial buildup in the hair follicles. The treatment for each condition can be different, so it is important to accurately diagnose the condition before starting treatment.